Want to experience the greatest in board studying? Check out our interactive question bank podcast- the FIRST of its kind here: emrapidbombs.supercast.com
Author: Blake Briggs, MD
Peer Reviewer: Mary Claire O’Brien, MD
Introduction
Ovarian torsion is a complete or partial rotation of the ovary against its ligamentous support, resulting in obstruction of its blood supply. It is in the top 3 most common female genitourinary emergencies; however, it can be elusive to diagnose for many reasons. Patients can have a variety of presentations, and their symptoms are often nonspecific. The traditional teaching on this disease is often mistaken as well. The actual incidence is unknown, but many reports emerging from various women’s hospitals and gynecologic acute care centers document that ovarian torsion is in the top 5 most common gynecologic emergencies. In another review of surgically treated adnexal mases, torsion accounted for 15% of cases.
Pathophysiology
The suspensory ligament of the ovary is the only ligamentous attachment to the ovary. It is otherwise not fixed. When torsion does occur, the ovary rotates around its ligament causing compression of the ovarian blood vessels and lymphatic vessels. Initially, venous flow is impaired, and depending on the severity of the compression, atrial flow compromise may follow.
Even blocking venous flow can result in ovarian engorgement with edema, resulting in ischemia.
There is no specific duration of time after symptoms that can predict irreversible tissue necrosis, but speed is always of the essence in diagnosis.
Accelerate your learning with our EM Question Bank Podcast
- Rapid learning
- Interactive questions and answers
- new episodes every week
- Become a valuable supporter
Risk factors
By far, the greatest risk factor is the presence of an ovarian mass and history of prior ovarian torsion. It is critical to note that normal ovaries can undergo torsion, but the presence of any mass is the greatest risk factor.
“Over 85% of patients with ovarian torsion have an ovarian mass.”
Let that one sink in for a minute. That’s a major statistic you need to remember. The larger the mass, the greater the risk. Torsion is most likely to happen if the size is >5 cm.
By mass, we don’t mean malignancy—it may be a physiologic cyst (functional, corpus luteum) or a benign tumor.
Due to physiologic cysts being more common, hormonal changes can greatly determine the risk of cyst size. Therefore, the risk of torsion is increased in women of reproductive age, women who are pregnant, and women with polycystic ovarian syndrome. Postmenopausal patients are at less of a risk.
Presentation
The traditionally taught presentation is acute, sudden onset of moderate to severe pain, usually localized to one side of the pelvis, associated with nausea and vomiting.
Unfortunately, this is rarely seen, and many of the above symptoms are seen in a variety of other pathologies.
Pelvic pain: 90% of patients. Usually sudden onset but can develop over a period of a few days. It can be described as dull, sharp, colicky, or however the patient wants- there is no specific character.
Nausea +/- vomiting: ~50-70%, nonspecific.
The exam is variable and not very helpful. As usual, the pelvic exam comes up short in terms of diagnostic sensitivity and specificity, but in sexually active female, it must be performed to assist in diagnosing other pelvic pathologies such as PID.
There are no laboratory tests that can help you.
Don’t go looking for a leukocytosis: it’s unreliable.
In summary, any female with moderate to severe lower quadrant abdominal pain or pelvic pain, consider ovarian torsion as a differential. It is less common than appendicitis or ectopic pregnancy, but cannot be ignored. Its presentation is quite variable, and one should have a low threshold to obtaining a transvaginal ultrasound.
Diagnosis
Perhaps the worst part of this pathology is that there is no gold standard imaging test in the ED.
The transvaginal ultrasound is good, but not great.
Positive findings vary, and may include the following:
-engorged, edematous ovary, with associated hemorrhage.
-Lack of Doppler flow
-“Whirlpool sign” (round hyperechoic structure with concentric hypoechoic stripes, thought to represent the twisting of the vascular pedicle).
While normal Doppler flow was once thought to exclude torsion, this is not the case. Perseveration of flow can occur due to incomplete torsion or intermittent torsion.
In general, the ultrasound sensitivity ranges from ~50-75%. Ouch. Not that comforting for your “go-to test” right?
The most sensitive ovarian findings are ovarian edema (85% sensitive, 18% specific), abnormal blood flow (85% sensitive, ~38% specific).
Pelvic MRI and CT are not routine imaging studies ordered for ovarian torsion. Yes, they may identify ovarian masses, but cannot perform Doppler flow analyses, and CT’s risk of radiation make it not an optimal test for torsion unless you are more concerned about other abdominal pathologies.
If you have an obviously positive ultrasound in the setting of a concerning patient presentation, then call gynecology for emergent laparoscopy. It is important you consider other pelvic pain mimickers such as ectopic pregnancy, intrauterine pregnancy, PID, and appendicitis.
If you have an indeterminant ultrasound but a concerning story and patient presentation, call gynecology anyway. The gold standard for diagnosis is laparoscopy.
One study showed that we as clinicians are quite bad at diagnosing ovarian torsion. In one series of 115 cases, the correct preoperative diagnosis was made in only 38% of cases. Ouch again.
Management
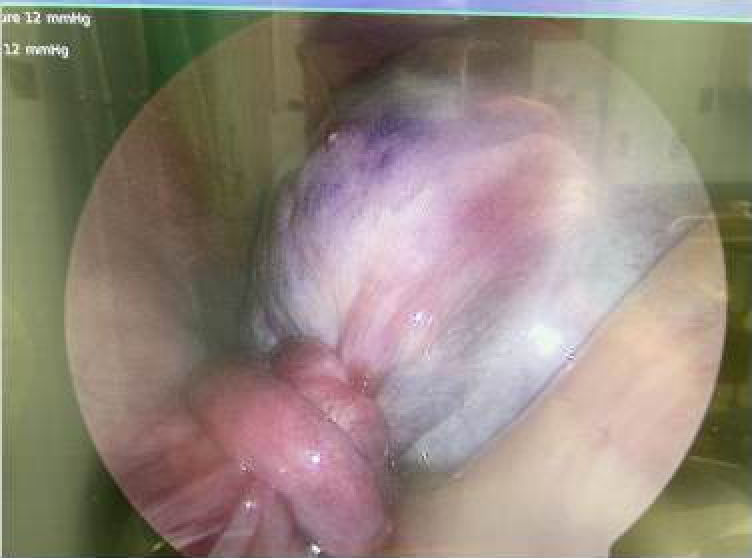
Laparoscopy with likely detorsion and preservation of the ovary. Ovarian necrosis is rare in most presentations, and therefore all ovarian torsion cases should be considered viable until proven otherwise in the OR.
Check out the photo here for what a positive finding is like. Scary.
References
- Sanfilippo JS, Rock JA. Surgery for benign disease of the ovary. In: TeLinde’s Operative Gynecology, 11th ed., Jones HW, Rock JA (Eds), Wolters Kluwer, 2015.
- Takeda A, Hayashi S, Teranishi Y, et al. Chronic adnexal torsion: An under-recognized disease entity. Eur J Obstet Gynecol Reprod Biol 2017; 210:45.
- Kokoska ER, Keller MS, Weber TR. Acute ovarian torsion in children. Am J Surg 2000; 180:462.
- Anders JF, Powell EC. Urgency of evaluation and outcome of acute ovarian torsion in pediatric patients. Arch Pediatr Adolesc Med 2005; 159:532.
- Hibbard LT. Adnexal torsion. Am J Obstet Gynecol 1985; 152:456.
- Bouguizane S, Bibi H, Farhat Y, et al. [Adnexal torsion: a report of 135 cases]. J Gynecol Obstet Biol Reprod (Paris) 2003; 32:535.
- Oltmann SC, Fischer A, Barber R, et al. Cannot exclude torsion–a 15-year review. J Pediatr Surg 2009; 44:1212.
- Varras M, Tsikini A, Polyzos D, et al. Uterine adnexal torsion: pathologic and gray-scale ultrasonographic findings. Clin Exp Obstet Gynecol 2004; 31:34.
- Houry D, Abbott JT. Ovarian torsion: a fifteen-year review. Ann Emerg Med 2001; 38:156.
- White M, Stella J. Ovarian torsion: 10-year perspective. Emerg Med Australas 2005; 17:231.
- SCHULTZ LR, NEWTON WA Jr, CLATWORTHY HW Jr. Torsion of previously normal tube and ovary in children. N Engl J Med 1963; 268:343.
- Cohen A, Solomon N, Almog B, et al. Adnexal Torsion in Postmenopausal Women: Clinical Presentation and Risk of Ovarian Malignancy. J Minim Invasive Gynecol 2017; 24:94.
- Anthony EY, Caserta MP, Singh J, Chen MY. Adnexal masses in female pediatric patients. AJR Am J Roentgenol 2012; 198:W426.
- Adnexal Torsion in Adolescents: ACOG Committee Opinion No, 783. Obstet Gynecol 2019; 134:e56.
- Argenta PA, Yeagley TJ, Ott G, Sondheimer SJ. Torsion of the uterine adnexa. Pathologic correlations and current management trends. J Reprod Med 2000; 45:831.



