Want to experience the greatest in board studying? Check out our interactive question bank podcast- the FIRST of its kind here: emrapidbombs.supercast.com
Author: Blake Briggs, MD
Introduction 1,2
Hyperkalemia is a common electrolyte issue seen in the ED. The three most common causes are: urinary retention, chronic kidney disease/ESRD, and drugs which raise serum potassium levels (see table to the right for common offending agents).
On a different note, “redistributive hyperkalemia” is seen in hyperglycemia such as HHS and DKA. In this form, hyperosmolarity and insulin deficiency cause potassium to move out of cells, but the total body amount of potassium is low due to dehydration.
This document will focus on hyperkalemic emergency, when prompt, immediate therapies are required.

Presentation
Patients may be asymptomatic or have nonspecific complaints (e.g. fatigue, weakness). Occasionally they have palpitations and chest pain. At high levels of hyperkalemia bradycardia is typically seen, with progression to slower heart rates, strange arrhythmias, and eventually poor end organ perfusion with subsequent change in mental status. Rarely, muscle weakness with paralysis can occur.
Determining urgency- the EKG 3
EKG and clinical features both the determine urgency of therapy. EKG should immediately be performed on all suspected hyperkalemic patients.
Accelerate your learning with our EM Question Bank Podcast
- Rapid learning
- Interactive questions and answers
- new episodes every week
- Become a valuable supporter
Hyperkalemia is the “lupus of EKG changes.” It can literally do whatever it wants.
Some examples include sinus bradycardia, slow idioventricular rhythms, ventricular tachycardia, any T wave changes, ST elevation, pseudo-Brugada pattern, and bundle branch blocks. Hyperkalemia is the most common electrolyte cause of cardiac arrest, and can cause asystole, PEA, ventricular fibrillation, and pulseless ventricular tachycardia. These are just a few of the classic changes that are frequently identified.
“When you see slow VT with rates <120, think hyperkalemia!”
There is a traditionally taught “order” of EKG changes, but we think its low yield for exams because in reality everyone knows the EKGs are variable and unpredictable. Just know the general theme:
Peaked T waves and shortened QT à progressive PR and QRS lengthening à disappearance of P wave, emergency of sine wave
Again, in reality the progression and severity of EKG changes do not correlate well with potassium concentration. See the example EKG to the right.
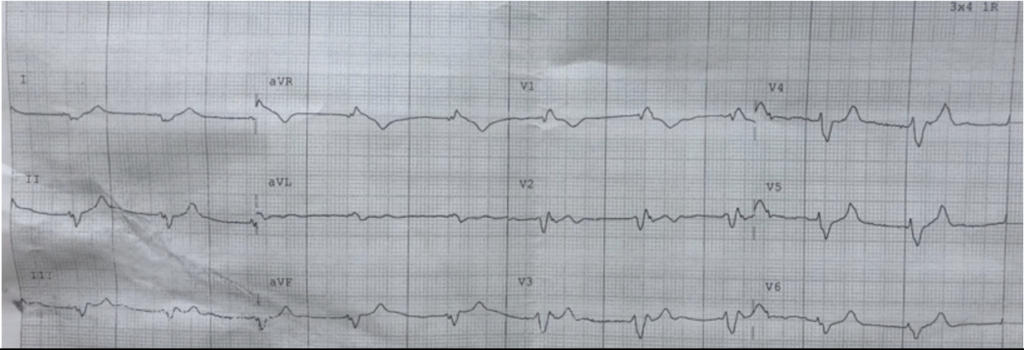
What is considered “hyperkalemic emergency”?
Hyperkalemic emergency is defined as patients with signs and symptoms of hyperkalemia, or EKG changes consistent with hyperkalemia. Patients tolerate acute hyperkalemia a lot worse than chronic hyperkalemia.
Other accepted definitions, with any one of the following being required:
– Any potassium level >6.5 mEq/L
– Moderate hyperkalemia (>5.5 mEq/L) with acute renal impairment, any crush injury, tumor lysis syndrome, or potassium absorption from GI bleeding
– Hyperkalemia in ESRD patients outside of regular dialysis
– Hyperkalemia in CKD patients not previously on dialysis but who have significantly higher potassium than normal
Who can have their potassium lowered slowly?
Asymptomatic patients with potassium level <5.5 mEq/L. These patients can be managed non-urgently by addressing the underlying cause such as dietary adjustments, cessation of causative medications, or optimizing chronic diseases which caused it (CKD, metabolic acidosis, etc).
Treatment of hyperkalemic emergency
All patients should be on telemetry. There are 3 types of therapies to treat hyperkalemic emergency: cardiac membrane stabilization therapy, therapies that drive potassium into cells, and therapies that excrete potassium. See the table to below for an outline on these therapies.
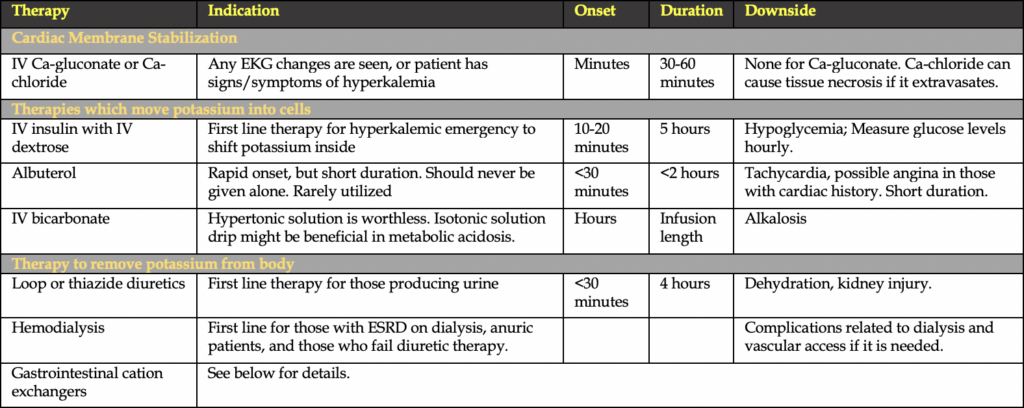
Cardiac Stabilization therapy 4,5
If EKG changes (discussed above) are seen: IV calcium. Calcium does nothing for potassium levels but stabilizes cardiac membranes by antagonizing potassium. It is fast (onset is within minutes), but short-lived. Its duration only lasts for 30-60 minutes, so reassessment of the patient is critical.
Available options: Ca-gluconate: 1g dose. Can be given through peripheral veins in a typical IV.
Ca-chloride: 1g. Contains three times the concentration of calcium, but should only be used if a central line is present, as its extravasation from peripheral lines can cause tissue necrosis. You may consider giving it via peripheral line or IO in a patient who presents in extremis or is pulseless, however there is no major evidence to support this. The reason you would be doing it is heroic efforts to save the patient and at the same time someone is obtaining central access. This is a discussion outside this review.
Therapies which move potassium into cells
Yes, there’s bicarbonate and albuterol, but these are not the “go-to” agents. They definitely should not be given instead of IV insulin.
IV insulin with IV dextrose 6,7,8: 10U regular insulin IV, 100 mL of 50% dextrose (50g of glucose). 5U should be used in those with renal insufficiency. This is the best medication to order for lowering potassium levels by driving potassium ions into the cell. The dextrose is given to counteract the insulin. Patients must undergo frequent hourly glucose checks up to 6 hours post-therapy as hypoglycemia occurs in 20% of patients.
Effects begin at 10-20 minutes, peaking in 30-60 minutes. They last for 5 hours which is very nice. Expect potassium to drop about 1 mEq/L. Patients will often require frequent re-dosing because as you attempt to remove potassium from the body it can take several hours or be delayed (e.g. setting up dialysis), so you need to stay on top of this!
Albuterol 9: 10-20 mg in 4mL saline nebulizer. That’s ~4-8 nebulizer treatments total (a LOT!). Peaks in 90 minutes, duration <2 hours.
Hypertonic bicarbonate ampules 10: No help. Hypertonic nature of the fluid pulls potassium out of cells.
Isotonic bicarbonate 10,11: limited efficacy only in metabolic acidosis. It must be given with an IV fluid drip as well typically at a rate of 150 mmol/L (D5W w 3 amps bicarbonate per liter). It helps lower potassium levels by dilution and alkalosis.
Therapies to remove potassium from body
First, determine if the patient is hypovolemic.
If the patient is hypovolemic and with metabolic acidosis: start a sodium bicarbonate drip along with lactated Ringers for resuscitation. LR does not cause hyperkalemia (11). Normal saline exacerbates hyperkalemia due to its acidotic nature.
Diuretics: high doses are usually needed with some combo of the following: Furosemide 80-120 mg IV or Bumetanide 2-4 mg IV, chlorothiazide 500 mg IV, and acetazolamide 500 mg IV. Keep dialysis as an option as you monitor urine output. If the patient produces adequate urine, give lactated Ringers and monitor electrolytes.
Hemodialysis 12: the only definitive method of reducing potassium levels. First line for those with ESRD on maintenance dialysis, anuric patients, and those who failed diuretic therapy.
What about gastrointestinal cation exchangers? 13, 14
Patiromer, sodium polystyrene (kayexalate), and zirconium cyclosilicate are often discussed as potential options, however their evidence is limited. For the most part, zirconium appears safe, but only lowers potassium by a little (0.2 mM in 12 hours) and may not be clinically relevant. It can be considered for use with loop diuretics.
We do not recommend ever giving kayexalate in the ED, and you can read this awesome Rebel EM article for more details. In particular, kayexalate is potentially harmful with rare cases of colonic necrosis, with basically NO evidence of lowering potassium levels urgently. Patiromer remains largely unknown, as there are no randomized controlled trials.
References
1. Mount DB. Disorders of potassium balance. In: Brenner and Rector’s The Kidney, 10th ed, W.B. Saunders & Company, Philadelphia 2015. p.559.
2. Kamel KS, Wei C. Controversial issues in the treatment of hyperkalaemia. Nephrol Dial Transplant 2003; 18:2215.
3. Littmann L, Gibbs MA. Electrocardiographic manifestations of severe hyperkalemia. J Electrocardiol 2018; 51:814.
4. Winkler AW, Hoff HE, Smith PK. Factors affecting the toxicity of potassium. Am J Physiol 1939; 127:430.
5. BRAUN HA, VAN HORNE R, BETTINGER JC, BELLET S. The influence of hypocalcemia induced by sodium ethylenediamine tetraacetate on the toxicity of potassium; an experimental study. J Lab Clin Med 1955; 46:544.
6. Ferrannini E, Taddei S, Santoro D, et al. Independent stimulation of glucose metabolism and Na+-K+ exchange by insulin in the human forearm. Am J Physiol 1988; 255:E953.
7. Pergola PE, DeFronzo R. Clinical disorders of hyperkalemia. In: The Kidney: Physiology and Pathophysiology, Seldin DW, Giebisch G (Eds), Lippincott Williams & Wilkins, 2000. Vol 2, p.1647.
8. Lens XM, Montoliu J, Cases A, et al. Treatment of hyperkalaemia in renal failure: salbutamol v. insulin. Nephrol Dial Transplant 1989; 4:228.
9. Liou HH, Chiang SS, Wu SC, et al. Hypokalemic effects of intravenous infusion or nebulization of salbutamol in patients with chronic renal failure: comparative study. Am J Kidney Dis 1994; 23:266.
10. Blumberg A, Weidmann P, Shaw S, Gnädinger M. Effect of various therapeutic approaches on plasma potassium and major regulating factors in terminal renal failure. Am J Med 1988; 85:507.
11. Blumberg A, Weidmann P, Ferrari P. Effect of prolonged bicarbonate administration on plasma potassium in terminal renal failure. Kidney Int. 1992 Feb;41(2):369-74.
12. O’Malley C, Frumento R, Hardy M, et al. A randomized, double-blind comparison of lactated Ringer’s solution and 0.9% NaCl during renal transplantation. Anesth Analg. 2005;100(5):1518-24, table of contents.
13. Nolph KD, Popovich RP, Ghods AJ, Twardowski Z. Determinants of low clearances of small solutes during peritoneal dialysis. Kidney Int 1978; 13:117.
14. Farkas, Josh. PulmCrit – Sodium Zirconium Cyclosilicate for urgent treatment of hyperkalemia. https://emcrit.org/pulmcrit/zirconium-cyclosilicate/. May 20, 2020. Accessed 10/23/20.
15. Swaminathan, Anand. Is Kayexalate useful in the treatment of hyperkalemia in the emergency department? https://rebelem.com/kayexalate-useful-treatment-hyperkalemia-emergency-department/. 2/2/2015. Accessed 10/23/2020.


